How Jet Fumes And Hypoxia On Planes Affect The Body

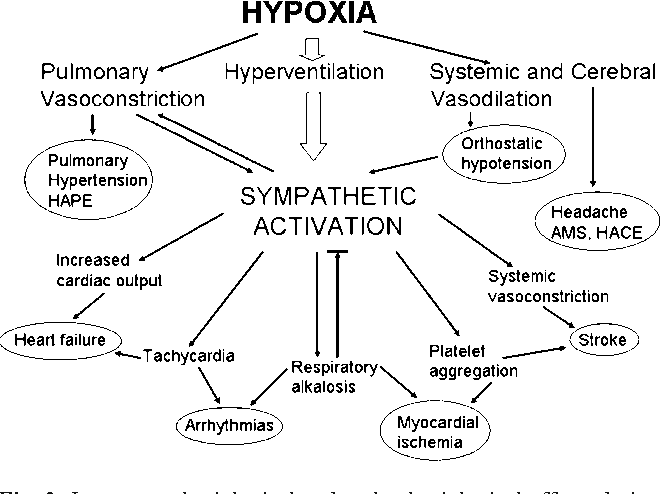
Hypoxia (loss of oxygen) is a major stressor on the body.
On average, one can live ~21 days without food, ~2 days without water, but only a few minutes without oxygen. R
Most studies review long term exposure of hypoxia, but in this post we will discuss what happens to the body on a cellular level when exposed to hypoxia in the short term, such as flying or space travel (in a non-hormetic way). R.
Basics
Almost two billion people use commercial aircrafts annually. R
When you go on a plane, you normally reach altitudes that cause hypobaric hypoxia (~2300m/8000ft). R
The higher you go into the atmosphere, air pressure (hypobaric) and oxygen (hypoxia) both become less available. R
This means there is less oxygen available to mitochondrial metabolism and less oxygen to saturate tissue, so the body must adapt to this stressor. R
This condition is called short-term hypobaric hypoxia (STHC) or intermittent hypobaric hypoxia (IHH) and as an adaptive response to keep to body in homeostasis, this creates proteopathy (misfolding of proteins). R R R
Hypobaric Hypoxia
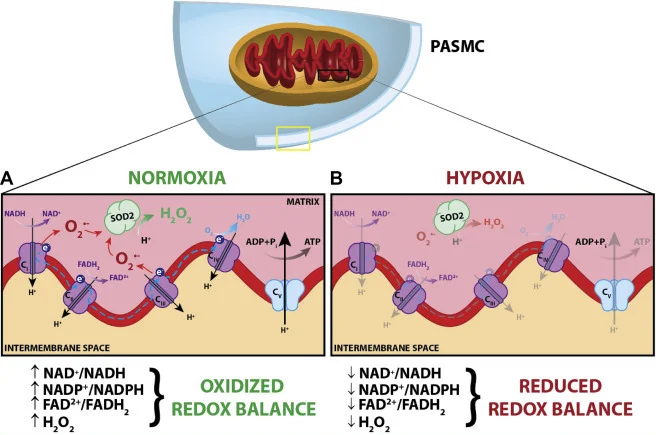
1. Starves Mitochondria
STHC causes mitochondria to produce more free radicals than it can quench. R
STHC limits the availability of oxygen for reduction to H2O2 at cytochrome oxidase. R
This leads to further production of ROS and RNOS. R
2. Reduces Cognitive Function And Brain Permeability
STHC may reduce cognitive function. R
STHC causes cognitive impairment (affecting memory function specifically) causing hippocampus mitochondrial and synaptic lesions. R
As seen in astronauts, STHC may induce with swelling of the optic disc due to disruption the blood-brain barrier (BBB) and result in cerebral edema. R
STHC in the brain and vascular system decreases expression of the gene Apo-E. R
This reduction in Apo-E makes it harder to protect against glutamate-induced cell death.R
Apo-E also has many effects such as antioxidant, anti-platelet aggregation, anti-proliferative effects, and immunomodulation properties. R R R R
3. Induces Headaches
Changes in cabin pressure during take-off and landing can cause airplane headache (AH). R R R
AH has been commonly associated with anxiety. R
CGRP and VIP levels may be decreased during AH (needs further research). R
4. Impairs Liver Function
STHC may induce insulin resistance as it reduces retinol binding protein (RBP4) which down-regulates GLUT4 (insulin-dependent factor that moves glucose into fat/muscle). R
This also releases more retinol (in free form) into the extracellular space of the cell (10x more than normal). R
In animal models, STHC has shown to increase gluconeogenesis in the liver. R
5. Increases Coagulation
STHC increases the risk of thrombosis. R R
This increases the risk of developing stroke, chronic obstructive pulmonary disease (COPD) and obstructive sleep apnea syndrome (OSAS). R R R
Flying (STHC) triggers systemic inflammation and platelet activation, which leads to coagulation induction and degranulation of platelets. R
Also, STHC reduces Apo-M (protects LDL from oxidative stress) and Apo-H (prevent activation of the intrinsic blood coagulation). R R
It may also make sickle cell disease worse as it causes sickling of blood cells. R
STHC increases hypoxia-inducible factor-1 and -2 (HIF1a and HIF2a) and causes iron dysregulation in the blood. R
6. Reduces Lung Function
Higher altitudes alter pulmonary function and may make respiratory conditions worse (such as COPD, asthma, pneumothorax, bronchogenic cysts, restrictive pulmonary diseases, cystic fibrosis and pulmonary hypertension). R
As an adaptive response in STHC, ApoA-I gene expression increases. R
ApoA-I protects arteries in the lungs, maintains airway function, and helps prevent inflammation and collagen deposition in the lung. R
7. Worsens Wound Healing
STHC reduces fetuin. R
Fetuin plays as an anti-inflammatory mediator that is critical to regulating the innate immune response following tissue injury. R
8. Damages Vision
STHC may cause optic neuropathy (OD). R
For example, in a case study, a 12 hour flight caused a patient to develop OD in the right eye. R
STHC may also induce myopia. R
For example, in another case study, a patient developed myopia in his right eye after a plane landing. R
9. Worsens Exercise Performance

Exposure to moderate altitude accelerates destruction of muscle tissue. R
It also increases the ability for muscles to become fatigued (as STHC accelerates the transition from the slow-to-fast-twitch fiber type and decreases mitochondrial function/aerobic metabolism in muscles). R
Training in hypoxia, Intermittent induced cyclic hypoxia (IICH), has been studied recently in athletes. R
IICH can stimulate erythropoietin and red blood cell production and increase ventilation. R
IICH may also increase arterial blood pressure through activation of the reninangiotensin system in healthy subjects. R
It also enhances sympathetic and blood pressure responses to acute hypoxia and hypercapnia. R
However, exercise with oxygen therapy (EWOT) + IICH does show some benefits (see separate post). R R
10. Decreases Immune Function
Reactivation of latent herpes viruses often occurs during short-duration flights. R
STHC suppresses the immune system - T cell function is impaired during hypoxic stress and promotes the accumulation of extracellular adenosine as a result of enhanced purine nucleotide degradation from adenosine tri- and diphosphate (ATP, ADP). R
11. Worsens Inflammatory Bowel Disease
Flying can cause Inflammatory Bowel Disease (IBD) flares. R
Crohn's Disease (CD) and Ulcerative Colitis (UC) patients have shown to have elevated levels of HIF-1α and HIF-2α. R R
12. Impairs Sleep And Jet-Lag Recovery
Flying with STHC may reduce the ability to sleep and make jet-lag symptoms worse. R
13. Alters Water Intake
STHC reduces water intake. R
Cabin Air
Jet Fumes, Cabin Air, And Aerotoxic Syndrome

Most human and animal studies show the effects of jet fumes to be pretty benign, but are not completely harmless. R
They have been linked to aerotoxic syndrome (ill-health effects caused by breathing contaminated/toxic airliner cabin air). R
Exposure to jet fumes in the respiratory system have shown to cause the production of phlegm, cough, and asthma. R
Studies have also shown that neurotoxins found in cabin air jet fumes have been linked cognitive impairment and loss in brain white matter. R R R
Also, long-term studies of US flight attendants show a possible link to:
Breast cancer - circadian disruption disrupts melatonin production and may worsen EMF radiation R
Neurodegeration - suggesting that flight attendants may have an increased risk of Amyotrophic lateral sclerosis (ALS) R
These fumes may get in via engine bleed, which is called a fume event - if an engine bearing seal fails and begins to leak, depending on the location of the seal, some amount of engine oil may be released into the compressed air stream. R
Jet fuel (such JP-8) and jet oil are commonly linked to aerotoxic syndrome and many chemicals from them can be inhaled including: R R R
Exposure to these chemicals may increase risk for developing cancer or other pathologies in humans who are occupationally exposed (such as air force, airport/airplane workers, and firefighters). R R R
Exposed flight-crew members have reported symptoms, including dizziness, nausea, disorientation, blurred vision, and tingling in the legs and arms. R
Cabin air also has flame retardants circulating from plane materials, which are known carcinogens. R
Carbon Dioxide
Recirculated air increases the amount of carbon dioxide (CO2). R
CO2 may: R
Alter behavioral health and performance - irritable, lethargic, visuomotor impairment, nausea, dizziness, derealization, fear of losing control, and paresthesia
Alter bone homeostasis - results in acidosis and the release of calcium carbonate and bone breakdown, so may cause kidney stones
Alter the binding of oxygen in blood - less O2 is bound to hemoglobin
Stimulate hyperventilation - has shown to cerebral blood flow (CBF) by up to 35%, without returning to baseline post-exposure
Vasodilate the brain
How To Protect Against Hypobaric Hypoxia
Check oxygen levels with a SpO2 meter (only represents blood oxygen, not cellular).
Lifestyle:
Hyperbaric Oxygen Therapy (possibly)
Wear Elastic Stockings / Compression Socks - May help prevent thrombosis during long flights R
Supplements:
Ginkgo Biloba -helps with HH adaptation R
Glutamine - protects from intestinal injury and regulates the gut flora imbalance in hypoxia environment R
Nitrates (or Neo40)- improves blood flow and is paramount if training (exercising) in hypoxia R R
Quercetin - helps improve brain/mitochondrial function via Sirt1/PGC-1α/FNDC5/BNDF R
Drugs:
Antihistamines - may help with airplane headaches (decreases sinus mucous) R
Pathways:
Hypoxia Tolerance
In humans, hypoxia tolerance improves with increased nitric oxide availability, so consuming greens or supplementing with nitrates may help improve tolerance. R
Another reason for eating greens (or meats) is to increase iron levels, which help with STHC adaptation. R
Also, hypoxia tolerant animal models shower higher levels of the following proteins, so upregulating their expression may be beneficial: R
Increase CRP
Increase CLC11
Increase GPx-3
Increase Hp
Increase PON1
Increase Rab-3D
Increase TTR
Reduce C3
Reduce C4
Mechanism Of Action
Hypobaric Hypoxia:
Increases AAT R
Increases Aldosterone R
Increases CLU R
Increases CRP R
Increases C1QA R
Increases C1QB R
Increases Enoyl CoA hydratase R
Increases F2 R
Increases GAPDH R
Increases GST-P1-1 R
Increases HBA R
Increases Hemopexin R
Increases HP R
Increases IL-6 R
Increases Myoglobin R
Increases NMDA R
Increases PAI1 R
Increases Prothrombin R
Increases Renin R
Increases sP-selectin R
Increases TAT R
Increases TTR R
Increases VDBP R
Reduces ALB R
Reduces Amyloid (serum) R
Reduces Apo-H R
Reduces CAT R
Reduces CA1 R
Reduces Cortisol R
Reduces C3 R
Reduces C4a R
Reduces Fetuin R
Reduces PGK1 R
Reduces RBP (plasma) R
Reduces Transferrin R
Jet Fumes
Genetics
FAM213A
rs77999529
Exhibits a low minor allele frequency in various human populations (may be beneficial for high-altitude adaptation studies have shown accelerated growth in lung volume and chest dimensions in highlanders vs. lowlanders, which might be a developmental compensatory response to high-altitude hypoxia) R
rs150230265
Exhibits significant allele frequency differences between highlanders vs lowlanders (may be beneficial for high-altitude adaptation studies have shown accelerated growth in lung volume and chest dimensions in highlanders vs. lowlanders, which might be a developmental compensatory response to high-altitude hypoxia) R
SFTPD
rs3923564
G allele - risk allele for chronic obstructive pulmonary disease R
rs7078012
T allele - risk allele for chronic obstructive pulmonary disease R
rs3088308
serine to threonine subsitution - damaging and exhibits significant differentiation between HL and LL R
rs721917
Thr/Thr genotype - had significantly lower SP-D serum levels, and is associated with increased disease-susceptibility R
Met allele - associated with defense to respiratory syncytial virus R
rs2243639
More Research
Reduces SpO2 levels may correlate with flight phobia (not well researched). R