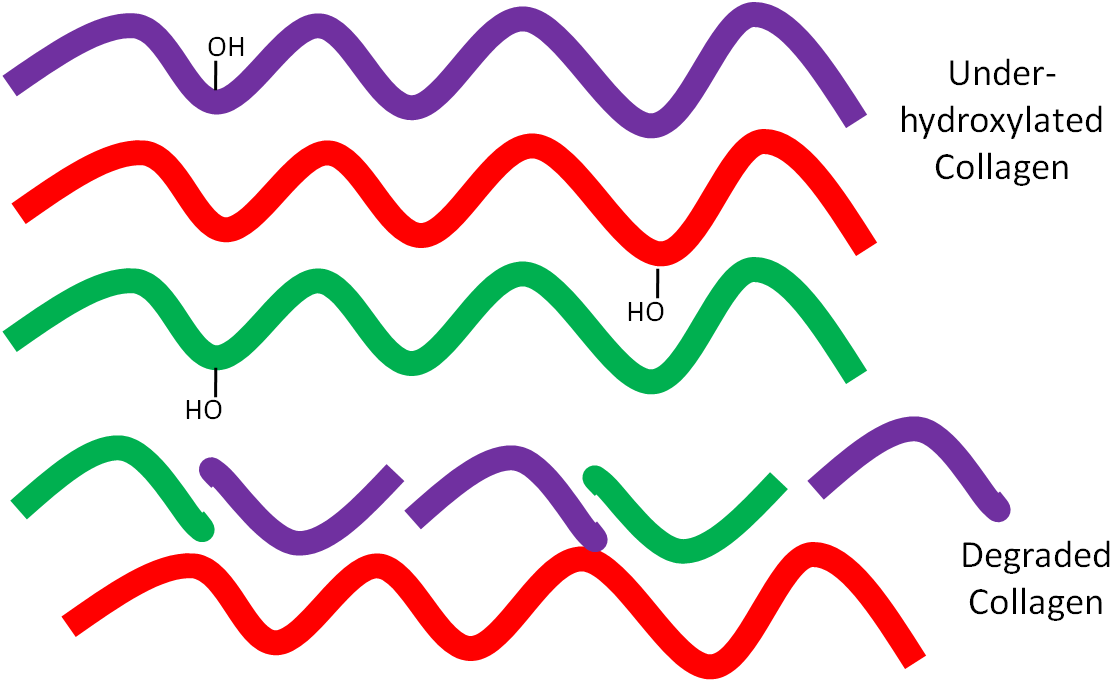
Why do I have a connective tissue disorder all of a sudden?
This is a great question, so let’s discuss!
Why COVID-19 can be more challenging for connective tissue disorder patients
Infections and the immune response:
During an infection, your immune system dispatches tools like phagocytes (cell eaters) and chemokines (signaling molecules) to the infected area. R R
These tools use hyaluronidase (HA-ase) and metalloproteinases (MMPs) to cut through the glycocalyx, a sugary layer on blood vessel linings and macrophages (immune cells). This allows them to reach pathogens and improve their binding efficiency. R R
The glycocalyx and connective tissue health:
The glycocalyx plays a vital role in regulating what enters and leaves cells. R R
It also sits above the extracellular matrix, a scaffold that includes collagen and other components essential for strong connective tissues (ligaments, tendons). R R
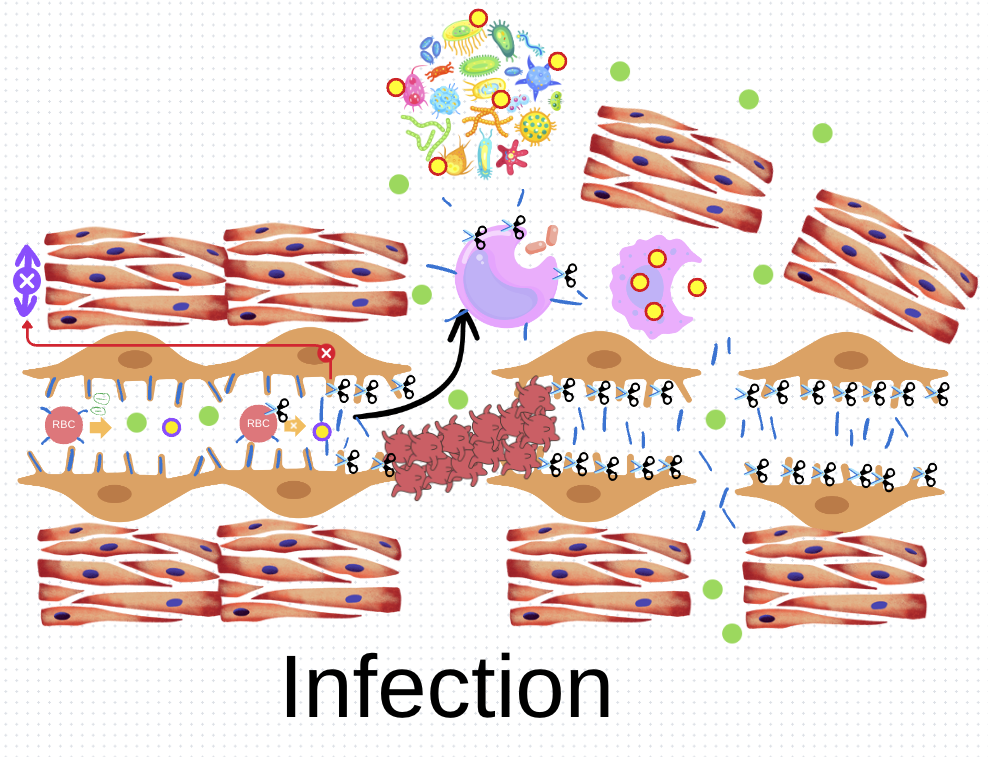
Double-edged sword: HA-ase, MMPs, and connective tissue damage:
Unfortunately, HA-ase and MMPs can also break down these very components, essentially degrading the glue that holds ligaments together. R R
COVID's spike protein and increased damage:
COVID-19's spike protein itself can damage the glycocalyx. R R
Additionally, the high levels of HA-ase and MMPs needed by phagocytes to clear away the SARS-CoV-2 virus and debris can cause significant collateral damage to connective tissues. R R
People with connective tissue disorders already have compromised connective tissue integrity. This additional damage from COVID-19 makes healing and recovery more difficult. R
Testing Connective Tissue
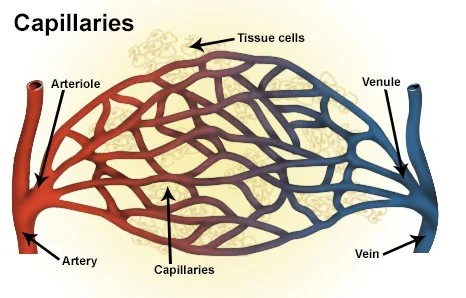
Capillary Networks
Tissues such as skeletal muscle, liver, and kidney have extensive capillary networks because they are metabolically active and require an abundant supply of oxygen and nutrients. R
Other tissues, such as connective tissue, have a less abundant supply of capillaries. R
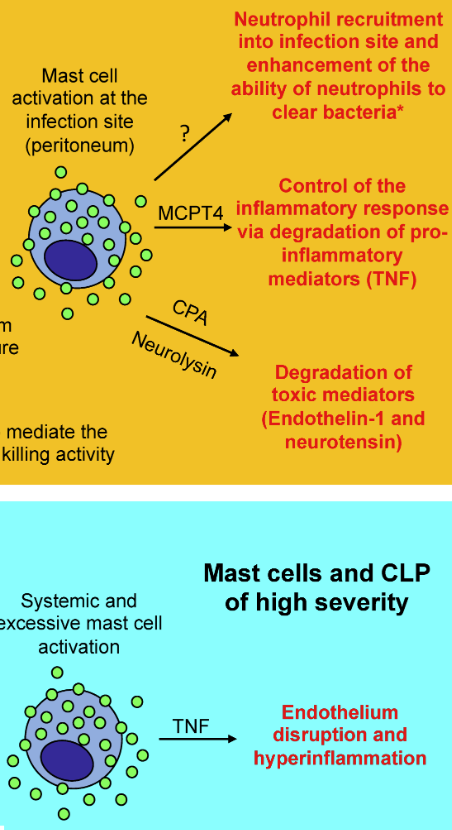
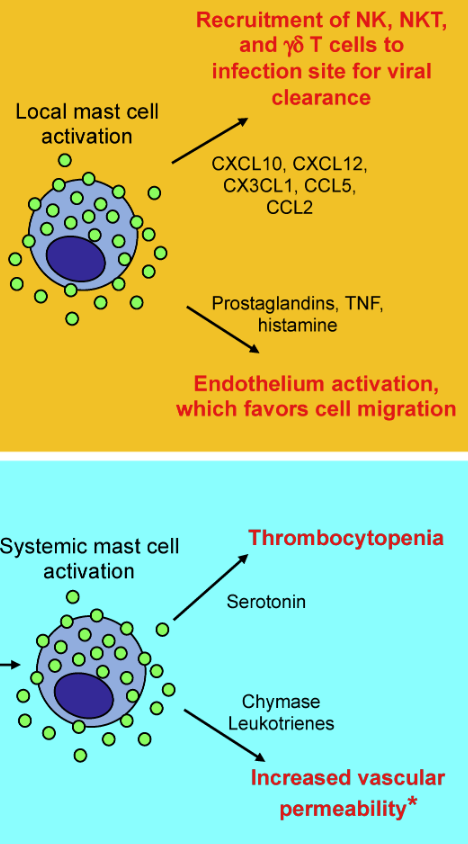
Mast Cells
Mast cells are classified as either connective tissue-type mast cells (CTMCs) or mucosal-type mast cells (MMCs). R
CTMCs typically reside in skin, the peritoneal cavity and many other locations, including the intestinal submucosa. R
In contrast, MMCs are predominant in the mucosal layer of the intestine, where their numbers expand dramatically during, for example, parasitic infection. R
Mast cells act as innate immune cells against pathogens and initiate defensive immune responses. R
Essentially, there are not a whole lot of capillaries to destroy in connective tissue, so if they get destroyed, then mast cells (get hypoxic and) try to re-oxygenate with histamine and mediators.
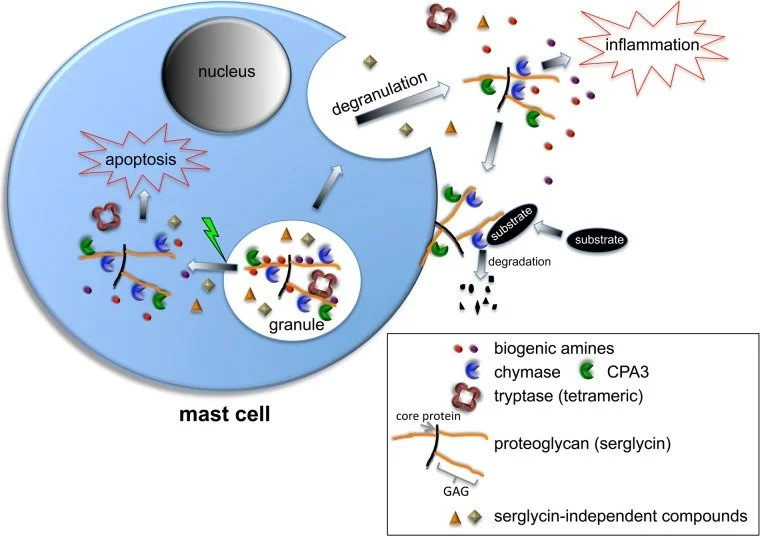
Connective Tissues and GAGs
Back to the connective tissue parts…
Your connected tissues are made up of glucosaminoglycans (GAGs) like glucosamine, and chondroitans like chondroitan sulfate.
Like discussed right above, in humans, both connective tissue mast cells and mucosal mast cells were found to contain GAGs with high affinity for antithrombin, when released can further degrade (and make it harder to repair) those connective tissues. R
Hypermobility and Vascular EDS
Vitamin C, lecithin, and collagen supplementation may help with this. R R
As Type IV EDS is a problem of the Extracellular Matrix remodeling, helpful tips can be found in my Extracellular Matrix Remodeling post. R
Thanks for reading!