Acute Inflammation
Acute inflammation is good.
This is tissue damage due to trauma, microbial invasion, or noxious compounds. R
It starts rapidly, becomes severe in a short time and symptoms may last for a few days. R
Subacute Inflammation
Subacute inflammation is the period between acute and chronic inflammation and may last 2 to 6 weeks. R
The problem is when you get stuck in chronic inflammation.
Chronic Inflammation Basics
This is slow, long-term inflammation lasting several months (to years). R
Generally, the extent and effects of chronic inflammation vary with the cause of the injury and the ability of the body to repair and overcome the damage. R
Some examples of chronic inflammation: R
Failure of eliminating the agent causing an acute inflammation such as infectious organisms including Mycobacterium tuberculosis, protozoa, fungi, and other parasites that can resist host defenses and remain in the tissue for an extended period.
Exposure to a low level of a particular irritant or foreign material that cannot be eliminated by enzymatic breakdown or phagocytosis in the body including substances or industrial chemicals that can be inhaled over a long period, for example, silica dust.
An autoimmune disorder in which the immune system recognizes the normal component of the body as a foreign antigen, and attacks healthy tissue giving rise to diseases such as rheumatoid arthritis (RA), systemic lupus erythematosus (SLE).
A defect in the cells responsible for mediating inflammation leading to persistent or recurrent inflammation, such as auto-inflammatory disorders (Familial Mediterranean Fever).
Recurrent episodes of acute inflammation - however, in some cases, chronic inflammation is an independent response and not a sequel to acute inflammation for example diseases such as tuberculosis and rheumatoid arthritis.
Inflammatory and biochemical inducers are causing oxidative stress and mitochondrial dysfunction such as increased production of free radical molecules, advanced glycation end products (AGEs), uric acid (urate) crystals, oxidized lipoproteins, homocysteine, and others.
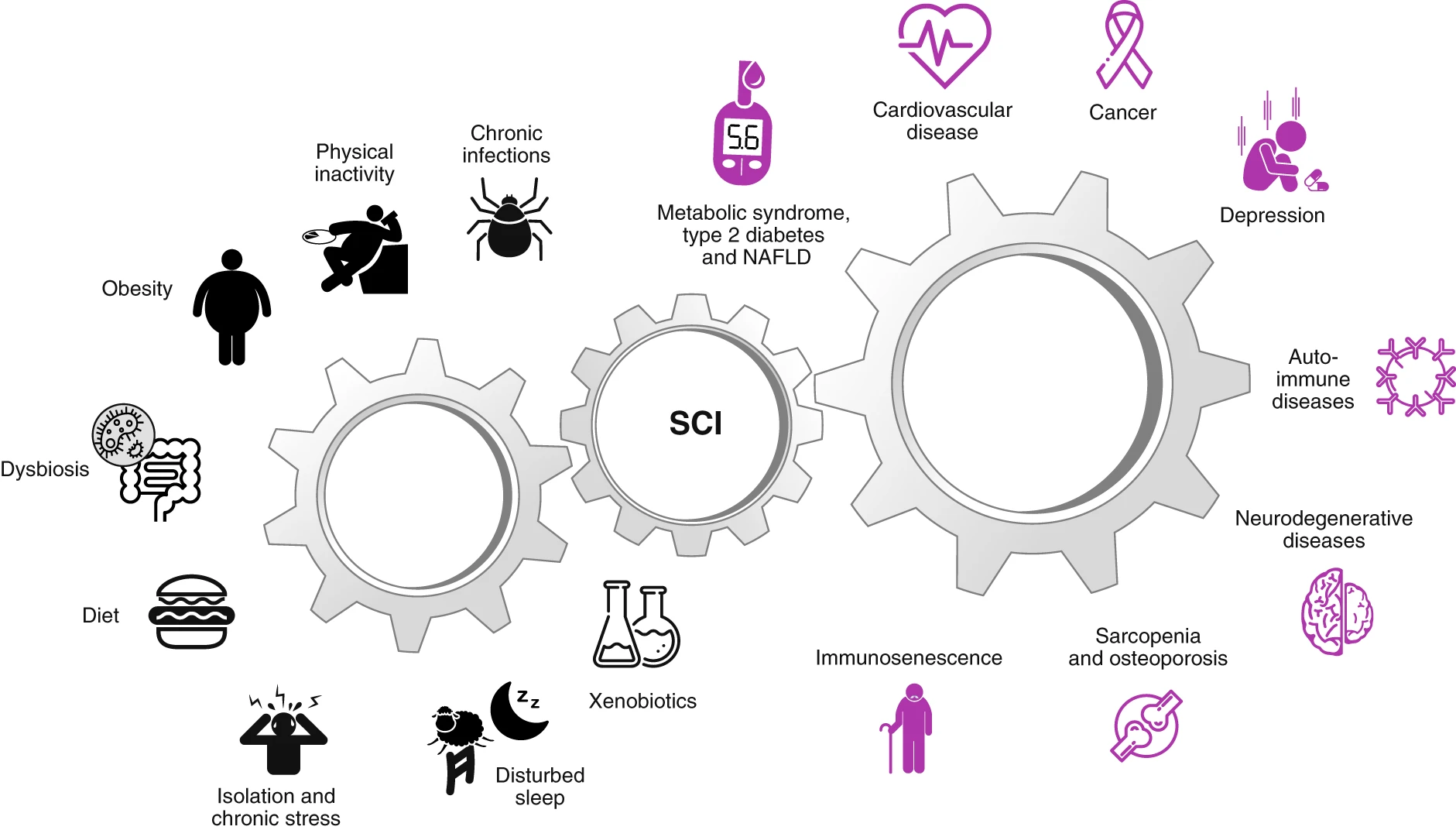
What Pathologies Are Stuck In Chronic Inflammation?
Some of the most common pathologies that keep you stuck in chronic inflammation (USA population based): R
Diabetes (9.4%)
Cardiovascular diseases (31%)
Arthritis and Joint Diseases (20%)
Allergies (8.2% of adults and 8.4% of children)
Chronic Obstructive Pulmonary Disease (COPD - 6.4%)
Cancers
Alzheimer's disease (AD)
Chronic kidney disease (CKD)
Inflammatory Bowel Disease (IBD)
Risk Factors and Symptoms Associated with Chronic Inflammation
Risk Factors
These are the most common (in the USA) risk factors associated with chronic inflammation: R
Age
Obesity
Diet
Smoking
Low Sex Hormones
Stress and Sleep Disorders
Symptoms
These are the most symptoms (in the USA) risk factors associated with chronic inflammation: R
Body pain, arthralgia, myalgia
Chronic fatigue and insomnia
Depression, anxiety and mood disorders
Gastrointestinal complications like constipation, diarrhea, and acid reflux
Weight gain or weight loss
Frequent infections
Best Tests for Chronic Inflammation
In my experience, the best tests to run for chronic inflammation as well as getting to actionable steps about those markers are with these tests:
More biomarkers from the literature:
I mean there are quite a ton of biomarkers, but they are likely downstream byproducts, not the root cause.
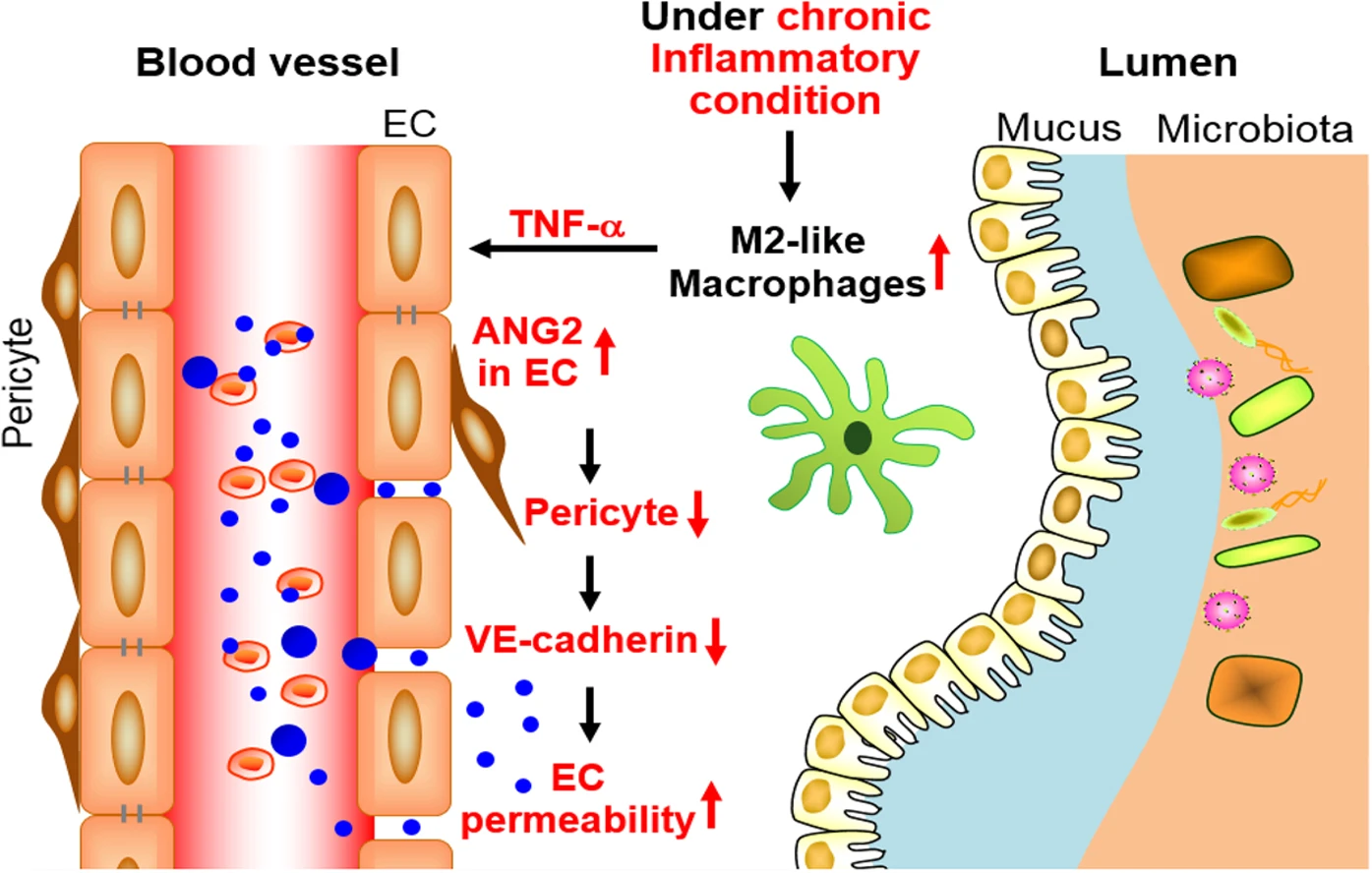
Chronic Inflammation in Junction Dysfunction
Chronic inflammation keeps those tight junctions open and thus keeps you leaky. R
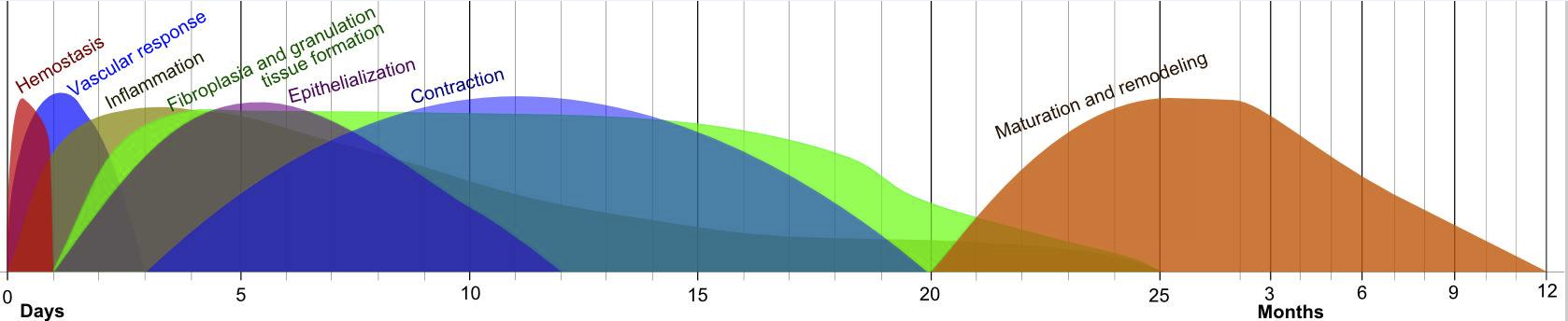
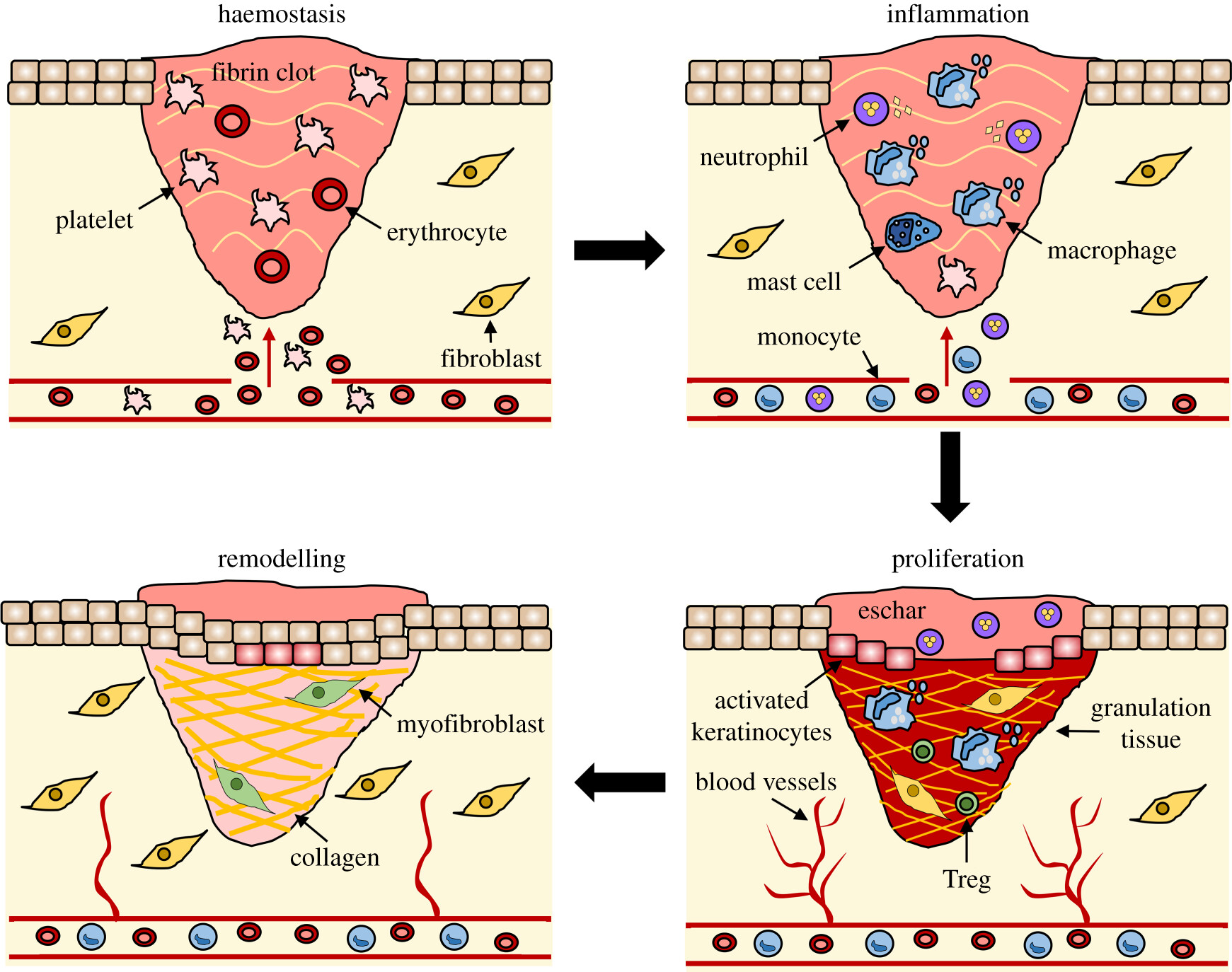
What Is The Wound Healing Cycle?
There are 3 degrees and 4 stages.
Most people with chronic inflammatory conditions (like post-viral illness) have chronic 3rd degree injuries thus get stuck in phases 1/2.
Simply put, this consists of: R
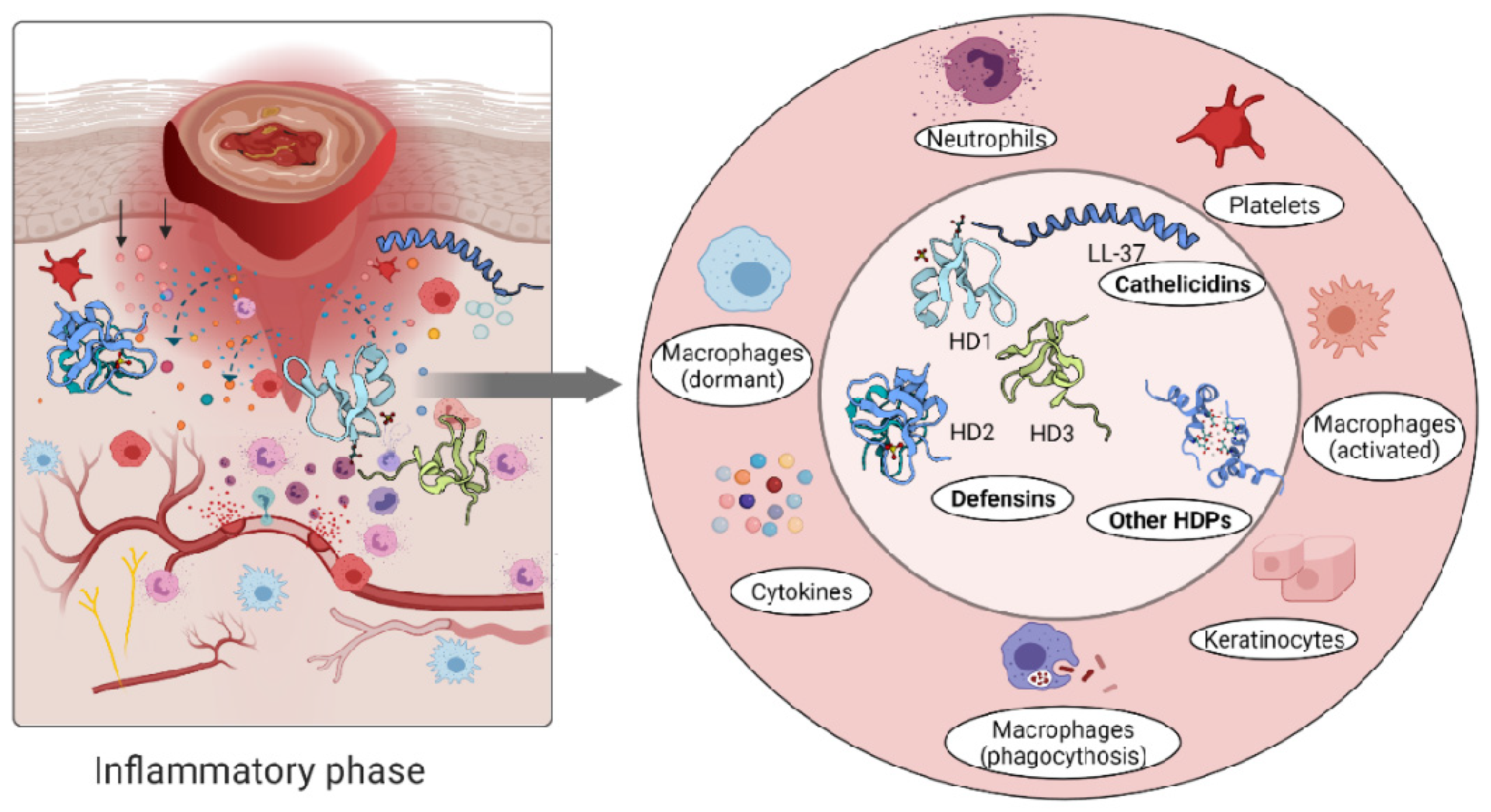
Release of ROS/RNS
Removal of debris and bacterial infection
Epithelial cells migrating toward wound sites
Some biomarkers in this phase include: R
LL-37
hBD-2
hBD-3
hBD-4
SR100a7
SPMs and hydrogen water are by far my two favorite ways to push the lever towards proliferation.
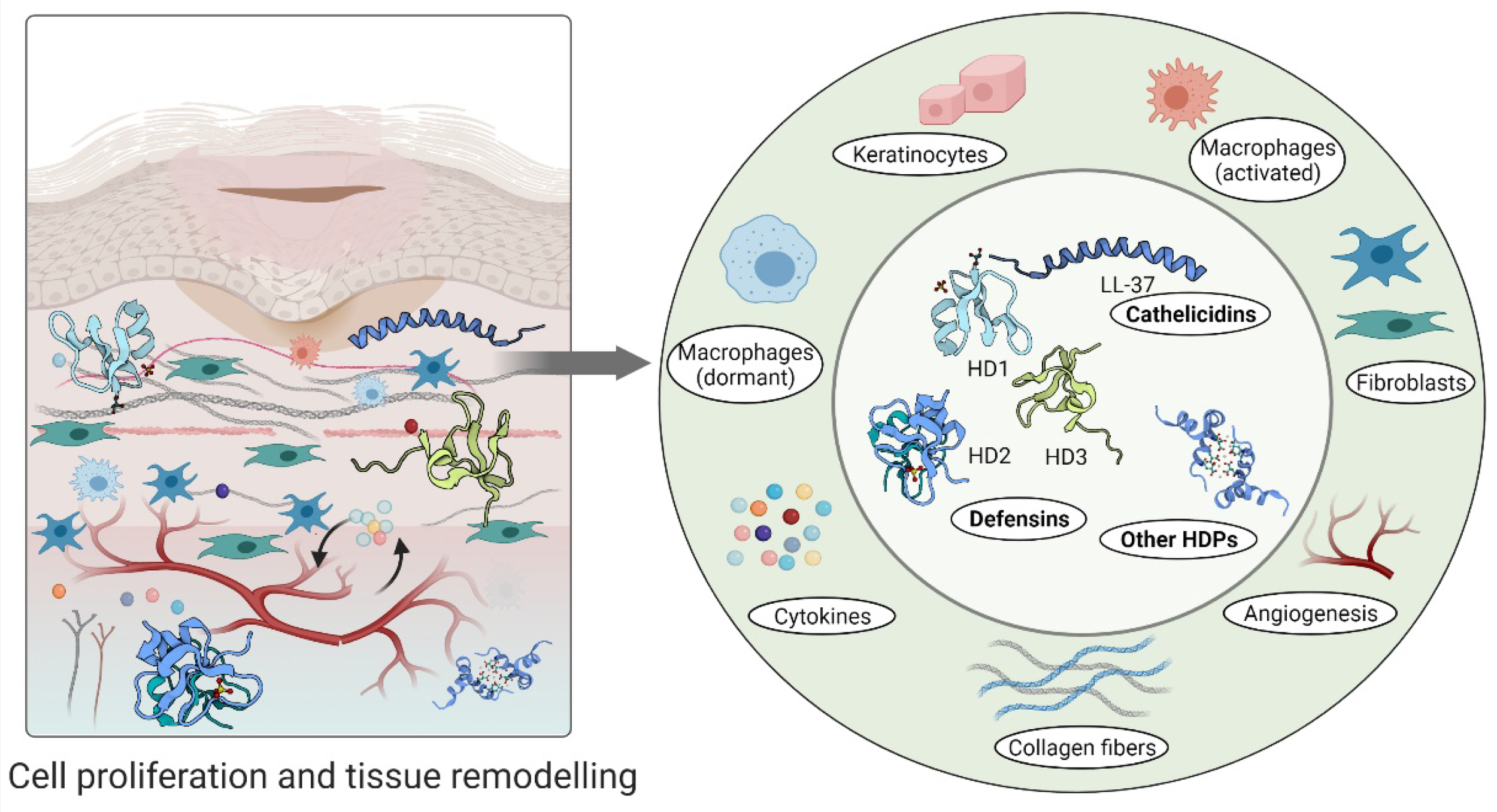
3) Proliferation
Simply put, this consists of: R
The wound completely covered by the formation of granulation
Some biomarkers in this phase include: R
LL-37
hBD-2
hBD-3
People with cancer may usually be stuck in this phase. R
4) Remodeling/Maturation
Simply put, this phase consists of: R
Fibroblasts cover the wound creating a new extracellular matrix (ECM)
The wound being completely closed
The scar matrix is formed
Some biomarkers in this phase include: R
LL-37
Cathelicidin-WA (CWA)
S100A7
Things To Stay Away From If Stuck In Chronic Hemostasis and Inflammation
Things that delay wound healing are:
repeated trauma
infections
necrosis (decreased blood supply)
These would be best to avoid:
Toxins (man-made materials, heavy metals, plastics, polymers, microbial toxins, etc) R
Eating plant toxins or opening up tight junctions (LPS and endotoxemia) R R
Lectins R
Alcohol R
Overeating R
Over Exercise R
Excessive Sun R
Smoking R
UVA (alpha-tocopherol can prevent the increase of IL-8) R
UVB R
Salmonella
Oxidative Stress R
Obesity R
Homocysteine R
Angiotensin II 1 Receptor agonists R
Moving From 1/2 To Wound Repair (3/4+)
What are some ways to bring inflammation down and turn on the next phases of wound healing?
Lifestyle:
Physical Exercise or Exercise Mimetics (if you have vasoadaptive capabilities) R
Fasting or Fasting Mimetics R
Sleep (see my sleep hacks and my zeitgebers post) R
Reduce Stress R
Meditation R
Sunlight (but not excessive)
Diet:
Caloric Restriction R
Low glycemic diet R
Reducing seed oils and oxidized fatty acids R
Flavanoids and Polyphenols from fruits and vegetables R
Fiber and Resistant starches R
Green and Black tea and their respective polyphenols/aminos (like EGCG and theanine) R R R
Unoxidized Sesame Oil (and their lignans) R
Modalities:
Supplements:
Turmeric (curcumin) - Tumero XL Active R R
Black Seed Oil (nigella sativa) R
Proteolytic Enzymes (Serratiopeptidase) or Fibrenza R
Fish Oil - Metagenics 1000 DHA EPA R
Hyssop R
Harpagophytum procumbens (Devil’s claw) R
Drugs:
Cannabinoids or terpenes (Linalool, B-Caryophyllene (BCP post), CBD, CBN, THC, and Limonene) R R
Sartans (like Losartan)
NSAIDs (not my favorite so read this post) R R
Corticosteroids R
There are a lot of other products and ways, but these are my favorite ways that I believe are the most actionable.